Do Vaginal Probiotics Actually Work? What 47 Clinical Trials Found
Your doctor might prescribe antibiotics for BV. Here is what they probably will not mention, recurrence can hit 50% to 80% within a year. New data shows the issue is not probiotics versus no probiotics. The issue is dead strains versus living strains with real biology.
Dr. Grace Holland
OB/GYN, Women's Health Researcher
Your doctor might prescribe antibiotics for BV.
Here is what they probably will not mention, there is a real chance it comes right back.
A 2023 review in Frontiers in Reproductive Health puts BV recurrence around 50% to 80% within 6 to 12 months after antibiotics.
Women do everything right, then end up in the same exam room again.
KEY WARNING
Recurrent BV is not a motivation problem. PMID 35416708 describes treatment failure near 50% in recurrent disease, with biofilms as a central reason.
The Counterintuitive Part Nobody Explains
People say probiotics are expensive placebos.
But although this sounds convincing, it misses the central issue, strain biology.
In fact, the question is not whether probiotics work.
The question is which strains are alive when they arrive, and which strains can produce active compounds in the vaginal environment.
KEY FINDING
Some probiotic strains behave like tiny drug factories. Others never make it past stomach acid. This gap explains why patient experiences look so different.
Harvard, October 2024, L. crispatus Makes Drug Like Molecules
A Cell Host & Microbe paper from the Smita Gopinath lab at Harvard T.H. Chan changed this conversation.
The team showed that Lactobacillus crispatus produces beta-carboline alkaloids with anti-inflammatory activity.
One metabolite, perlolyrine, reduced genital herpes disease scores in a mouse model.
Why does this matter for BV? Because it proves a vaginal commensal can secrete pharmacologically active compounds, not just passively occupy space.

The Biofilm Problem Nobody Talks About
Remember earlier, recurrence stays high even after symptom relief.
You see, antibiotics often clear planktonic bacteria first.
Biofilm bacteria can remain attached to tissue inside a protective extracellular matrix.
Persister cells inside this matrix survive, then reactivate after therapy stops.
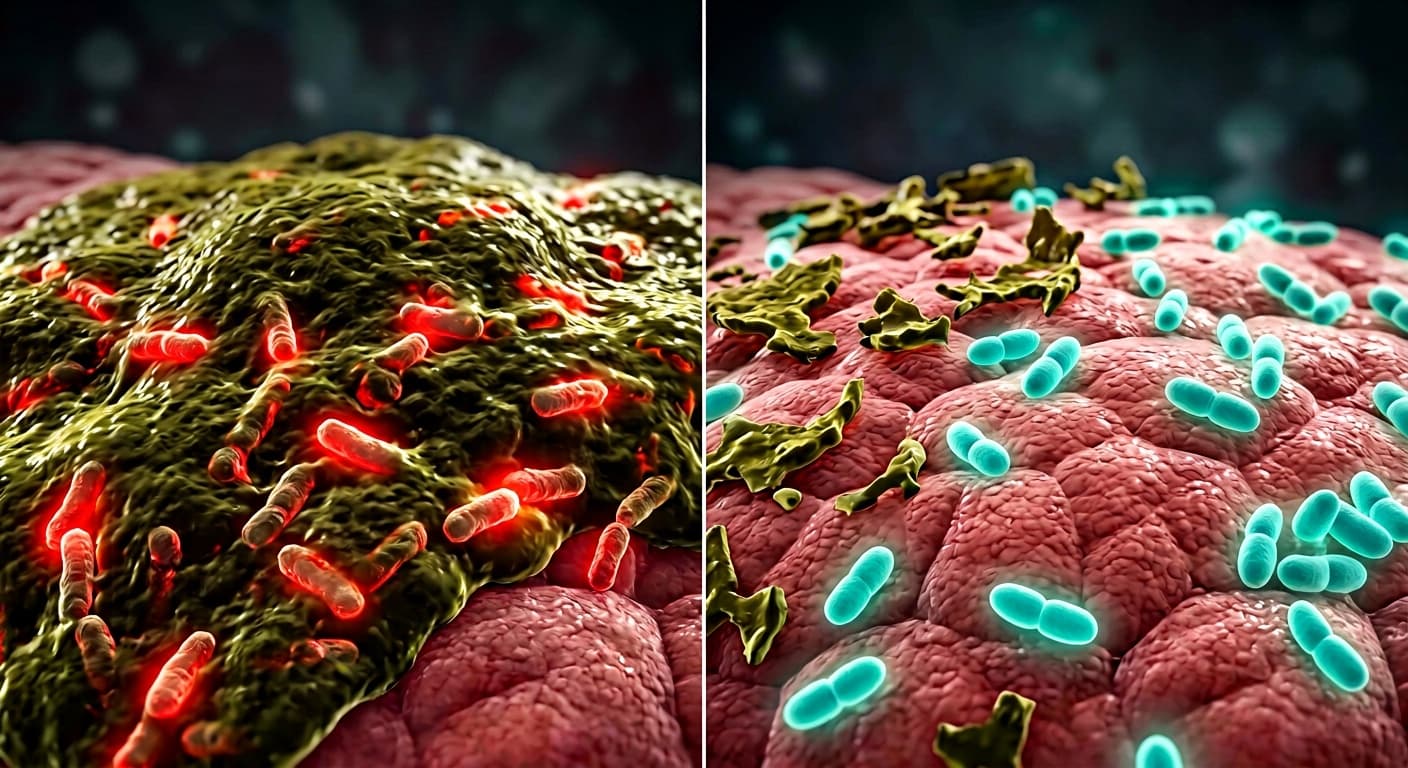
KEY WARNING
The more mature the biofilm, the more difficult recurrence control becomes. This is why short antibiotic cycles often fail in chronic cases.
Spore Forming vs Standard Probiotics
Did you know that gastric pH can drop into the 1.5 to 3.5 range.
Standard Lactobacillus capsules can lose most viability in this environment, with some products reporting losses near 99% before they reach the intestines.
Spore-forming strains, including Bacillus coagulans, carry a protective endospore shell and can show greater than 95% survival in simulated GI transit models.
Standard Lactobacillus Blend
- Acid sensitive in low pH environments
- Large viability drop before gut colonization
- Label CFU often overstates delivered CFU
Spore Forming Bacillus Strategy
- Protective endospore shell in gastric acid
- Higher delivery to the gut ecosystem
- More stable during storage and transit
Why Enzymes Change the Equation
Biofilm matrix is built from proteins, polysaccharides, and extracellular scaffolding.
Proteolytic enzymes such as bromelain can help degrade protein-rich parts of this matrix.
Why? Because once the shield weakens, antimicrobials and protective strains gain better access.
Early combination protocols suggest enzyme plus probiotic strategies can outperform single mode approaches in recurrence control.
KEY FINDING
Enzyme support does not replace antibiotics in active infection. It may improve follow-through by reducing biofilm persistence while probiotics rebuild Lactobacillus dominance.
What to Look For in a Probiotic That Actually Works
Most labels hide the details that matter most.
Use this quick screen before buying anything.
- Named strains, not generic species only. Look for identifiers like GR-1, RC-14, or CTV-05.
- Delivery logic. If oral, check survivability claims and whether CFU is guaranteed at expiration.
- Evidence for oral to vaginal impact. Multiple RCTs report that oral protocols can shift vaginal microbiome composition.
- Protocol fit. The more recurrent your BV pattern, the more you should discuss biofilm strategy with your clinician.
RED FLAGS
Skip products that hide strain names, promise instant cure language, or rely only on massive CFU numbers without viability data.
VERDICT
Do vaginal probiotics work. Yes, when they are the right strains, alive at delivery, and paired with a plan that addresses biofilm persistence. The issue is not probiotics versus placebo. The issue is biological precision versus generic blends.
FAQ
Do vaginal probiotics actually work?
Yes, specific strains can work. Multiple trials show better symptom control, improved vaginal pH, and lower BV recurrence when strain, dose, and timing are correct.
How long does it take for vaginal probiotics to work?
Most studies report measurable changes in 2 to 8 weeks. Recurrence prevention studies usually track 3 to 6 months.
Can you take probiotics orally for vaginal health?
Yes. Oral Lactobacillus protocols have shown vaginal microbiome changes and BV benefit through the gut-vaginal axis in randomized trials.
Why does BV keep coming back after antibiotics?
Biofilms and persister cells can survive therapy, then reseed infection when drug pressure stops. Loss of protective Lactobacillus also raises recurrence risk.
What is the best probiotic strain for vaginal health?
There is no single best strain for everyone. The strongest human evidence often centers on L. rhamnosus GR-1 with L. reuteri RC-14 orally, and L. crispatus for vaginal recolonization.
Sources
- Nwonu C, et al. "Lactobacilli as fungal safeguards in the female genital tract." Cell Host & Microbe, October 2024. PMID: 39423813. Read study.
- Castro J, Rosca AS, Cools P, et al. "Bacterial vaginosis recurrence rates and the vaginal microbiota, a review." Frontiers in Reproductive Health, 2023. Read review.
- Chan D, et al. "Vaginal microbiota and pharmacomicrobiomics. What do we know?" Frontiers in Cellular and Infection Microbiology, 2022. PMID: 35416708. PubMed.
- Reid G, et al. Oral probiotic lactobacilli and vaginal flora outcomes in women with recurrent BV. FEMS Immunology & Medical Microbiology, 2003. PMID: 12743835. PubMed.
- Anukam KC, et al. Oral Lactobacillus therapy in BV, randomized controlled trial. Microbes and Infection, 2006. PMID: 16697231. PubMed.
- Bonyar A, et al. Probiotics and recurrent bacterial vaginosis, systematic review and meta-analysis. Archives of Gynecology and Obstetrics, 2022. PMID: 36204368. PubMed.
Medical Disclaimer: This article summarizes published research and does not provide individual medical advice. If you have recurrent BV, work with your OB/GYN to build a treatment plan that fits your history.